Author: Dr John Maa University of California San Francisco 2008-07-29
Gallbladder disease: Symptoms, diagnosis, and intervention with cholecystectomy
Gallbladder disease: Symptoms, diagnosis, and intervention with cholecystectomy
Introduction
The gallbladder is a small, pear shaped organ adherent to the undersurface of the liver, whose purpose is to store bile produced by the liver to assist in digestion. While gallstones are very common, the majority of patients with gallstones are asymptomatic during their life, with only 1 to 2 % developing symptoms each year (1). The incidence of gallstones increases with age, and by the age of 70 approximately 20% of Americans have gallstones. Many patients are discovered at autopsy to have stones which were silent throughout their lifetime.Cholecystectomy is the surgical removal of the gallbladder. Gallbladder removal is performed most commonly to treat abdominal pain, or to remove an infected gallbladder and relieve complications of gallstone disease. Surgical removal of the gallbladder is one of the most common operative procedures performed in America, with an estimated 500,000 cholecystectomies performed annually (2). Approximately 6000 deaths annually result from gallstones or complications from treatment.
History of Gallbladder Surgical Techniques:
Carl Langenbuch of Germany was credited with performing the first elective open cholecystectomy in 1882 (3). Previous initial efforts to remove the gallstones and leave the gallbladder intact were unsatisfactory as surgeons soon recognized that the stones very often reformed. In an open cholecystectomy, the abdomen is incised approximately 20 cm to allow the surgeon to separate the gallbladder from its attachments to the liver and intestine by hand. For more than a century, open cholecystectomy has been the standard method of treatment of stone disease of the biliary system, with 95% of patients substantially relieved or cured of their symptoms.The first laparoscopic cholecystectomy was performed in Europe in 1987, and this minimally invasive approach to removal of the gallbladder has undergone rapid acceptance and growth worldwide (4). Laparoscopic cholecystectomy has now replaced open cholecystectomy as the first-choice of treatment for gallstones. In the laparoscopic (minimally invasive) approach, the gallbladder is removed using instruments and a video camera inserted through four incisions each less than 1 cm in size. The primary advantages are reduced postoperative pain, a shortened hospital length of stay, and a shortened time of recovery. Laparoscopic cholecystectomies can often be performed on an outpatient basis, with many patients able to return to work within the next few days.
The surgical approaches and indications for the open approach and the laparoscopic approach are discussed below.
In 2007, a new procedure, which avoids any visible external scars was reported (5). The gallbladder is removed through a transvaginal approach; as of early 2008 this type of natural orifice transluminal endoscopic surgery (NOTES) is still considered experimental and has not been widely adopted.
What is the role of the gallbladder?
Between meals, the gallbladder stores and concentrates bile produced in the liver, which assists in the digestion and absorption of food (especially fats). The gallbladder can hold approximately 50 mL of bile when fully distended (6). The gallbladder is connected by the common bile duct to the liver and small intestine (duodenum). When food is consumed, especially fatty foods, the gallbladder contracts and forces bile out of the ducts into the duodenum.Many patients question whether the gallbladder can be preserved during cholecystectomy, and wonder whether there are any long term effects after removal of the gallbladder. In the absence of a gallbladder for storage, bile is continuously secreted by the liver into the duodenum. This may result in mild diarrhea, which typically resolves within a few months after surgery (7). Experience has shown that stones will likely reform if the gallbladder is not completely removed.
Why do gallstones form?
There
are three types of gallstones: 1) cholesterol , 2) pigment, and 3)
mixed (both cholesterol and pigment). In the United States,
approximately 75% of gallstones are cholesterol, and the remaining 25%
are either pigment or mixed stones.
 |
| Cholesterol stones |
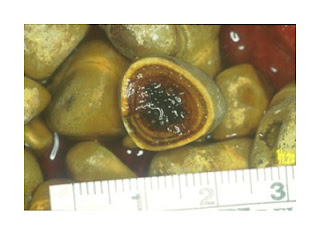 |
| Mixed stones |
The mechanism by which cholesterol stones form is not fully understood, but are likely the result of a complex alteration in hepatobiliary function. Cholesterol gallstones result from the secretion by the liver of bile supersaturated with cholesterol. This results in cholesterol crystallization and stone growth within the gallbladder, which can be exacerbated by gallbladder stasis. Most stones originate in the gallbladder and travel distally into the common duct; however, if the common bile duct is partially obstructed, stones can form there as well.
Pigment stones form by a different mechanism involving bilirubin degradation, and account for 25% of gallstones in the USA (and 60% of those in Japan). Pigment stones are black or dark brown, and are a mixture of calcium bilirubinate, bile acids, and bilirubin polymers. These stones are more common in Asians, and are more likely to involve bacteria in their development.
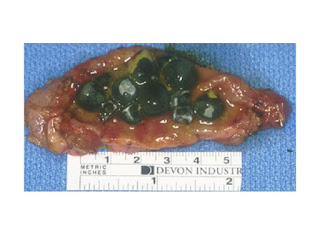 |
| Pigment stones |
What are the risk factors for forming gallstones?
1) Increasing age- stone formation is a time-dependent process2) Female gender—(female to male ratio is 3:1) it is believed that estrogen induces changes in lipid metabolism and gallbladder function – the risk is increased after having multiple children and use of oral contraceptives
3) Race and ethnicity- more than 75% of American Indian women over age 40 are affected
4) Genetics—increased risk if parents, siblings, or first degree relatives have gallstones
5) Obesity- a result of alterations in lipid metabolism and increased cholesterol synthesis due to increased activity of hydroxy-methyl-glutaryl- CoA (HMG CoA) reductase
6) Crohn's disease- due to decreased ileal resorption of bile salts
7) Total parenteral nutrition-which results in gallbladder stasis and distension
8) Rapid weight loss- approximately 30 to 40% of patients who undergo gastric bypass will form stones postoperatively, thus many surgeons recommend removal of the gallbladder prophylactically at the time of bariatric surgery
Why do gallstones cause problems?
Gallstones are most commonly located within the gallbladder, but can also be found within the common bile duct, liver, or in the intestinal tract, where they can cause life-threatening disease.The most benign form of gallstone disease is pain in the upper abdomen known as biliary colic. This is caused by transient gallstone obstruction of the cystic duct. The pain begins abruptly and then subsides, lasting for a few minutes to several hours. It is often associated with the ingestion of food, particularly fatty foods, but can occur spontaneously at any time. Elective surgery can be considered if biliary colic is poorly controlled with medications and interferes with quality of life.
More serious situations arise if a gallstone becomes impacted in the neck of the gallbladder, leading to infection and inflammation known as acute cholecystitis, which may lead to gangrene (gangrenous cholecystitis) and perforation of the gallbladder wall (leading to abscess or peritonitis). Gallstones that escape from the gallbladder and pass into the common bile duct (a condition known as choledocholithiasis) can cause other potentially severe complications such as obstructive jaundice, gallstone pancreatitis, and ascending cholangitis. When the gallbladder becomes adherent to the duodenum, colon, jejunum, or stomach, a cholecystenteric fistula can form. A gallstone that passes through the fistula may impact at the terminal ileum, causing a small bowel obstruction known as gallstone ileus. Surgery is often required, either urgently or after stabilization, for these complications of gallstone disease.
What are the symptoms of biliary colic?
Many patients develop some or all of the following symptoms:1) Sharp pains in the upper abdomen, especially on the right side
2) Frequent bouts of indigestion, especially after consuming fatty or greasy foods
3) Nausea, heartburn and bloating
Simple biliary colic, in the absence of gallbladder wall pathology or common bile duct obstruction, does not result in abnormal laboratory tests or abnormal vital signs.
What are the signs and symptoms of acute cholecystitis?
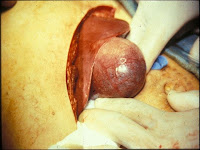 The
diagnosis of acute cholecystitis is based on the key findings of right
upper quadrant tenderness, fever, and leukocytosis. It is important to
distinguish biliary colic from acute cholecystitis, because
laparoscopic cholecystectomy is significantly more challenging due to
inflammation and adhesions around the gallbladder, edema, and friable
tissues which are more likely to bleed.Fully
80% of cases of acute cholecystitis result from stones (calculi)
causing cystic duct obstruction and secondary bacterial invasion. Many
of these cases will resolve on their own if the obstruction is relieved.
However, acute cholecystitis can also occur in the absence of stones—a
condition known as acalculous cholecystitis (10-20%), which can progress
more rapidly to gangrene and sepsis. This variant can result from
obstructing tumors or inadequate blood supply, and is seen more
frequently in patients with coronary artery disease, trauma, and
immunosuppression.
The
diagnosis of acute cholecystitis is based on the key findings of right
upper quadrant tenderness, fever, and leukocytosis. It is important to
distinguish biliary colic from acute cholecystitis, because
laparoscopic cholecystectomy is significantly more challenging due to
inflammation and adhesions around the gallbladder, edema, and friable
tissues which are more likely to bleed.Fully
80% of cases of acute cholecystitis result from stones (calculi)
causing cystic duct obstruction and secondary bacterial invasion. Many
of these cases will resolve on their own if the obstruction is relieved.
However, acute cholecystitis can also occur in the absence of stones—a
condition known as acalculous cholecystitis (10-20%), which can progress
more rapidly to gangrene and sepsis. This variant can result from
obstructing tumors or inadequate blood supply, and is seen more
frequently in patients with coronary artery disease, trauma, and
immunosuppression. With both calculous and acalculous cholecystitis, patients may develop the following symptoms:
1) Right upper abdominal tenderness--When the gallbladder becomes inflamed, pain will be triggered by touch-this is known as "Murphy's sign" as the patient abruptly stops breathing in when the gallbladder is palpated.
2) Fever– A temperature of 38 to 38.5 degrees centigrade often results from bacterial contamination of the biliary system.
3) Leukocytosis (an elevation of the white blood cell count) to 12,000- 15,000 cells per cubic millimeter (cmm).
4) Mild icterus: in 10% of cases, when the serum concentration of bilirubin rises above 2.5 mg/dl, a yellowish discoloration of the sclera becomes evident (icterus).
What are the complications of acute cholecystitis:?
Acute cholecystitis can also progress to more serious complications, which are the consequence of gallbladder ischemia and gangrene. The process begins as a sterile inflammation but quickly progresses to infection with E coli, Klebsiella, and enterococcus bacteria. The death rate rises to approximately 5%, which occurs more commonly in patients over 60 and diabetics, and often as a result of cardiovascular complications. Perforation can occur when an ischemic region of the gallbladder wall becomes necrotic (a condition known as gangrenous cholecystitis). If the perforation is walled off by adjacent omentum (a fold of tissue connecting to the liver) or other organs, a pericholecystic abscess can form.The major complications of acute cholecystitis which require prompt intervention are:
1) Empyema (suppurative cholecystitis), the gallbladder becomes filled with pus, and the patient has higher fevers to 39-40C, and a white blood cell count of about 15,000 cmm.
2) Perforation of the gallbladder, which can present as either a pericholecystic abscess and palpable mass, free perforation if the omentum does not wall off the process (1-2%), or a fistula to adjacent intestine
3) A severe and rare form of very severe infection of the gallbladder is known as emphysematous cholecystitis. It results from an anaerobic infection (clostridia or e. coli) with gas formation in the gallbladder wall and requires urgent intervention/surgery (often an open cholecystectomy).
What is ascending cholangitis?
Bacterial infection of the biliary tree signifies biliary obstruction, which can be caused by choledocholithiasis, biliary stricture, and tumors. The symptoms of cholangitis (known as Charcot's triad) are right upper quadrant pain, fever, and jaundice (a yellowing of the skin noted when the bilirubin level rises above 5 mg/dl). In the more severe form known as Reynold's pentad the additional findings of hypotension and mental status changes are noted. These conditions require clearance of the common bile duct, and are typically treated with intravenous antibiotics and endoscopic retrograde pancreatogram (ERCP), rather than cholecystectomy.
Which imaging studies can help diagnose gallstones and their complications?
The most useful test to diagnose gallstones is an ultrasound, which is a painless procedure that uses sound waves to detect stones. Ultrasound has both high specificity (> 98%) and sensitivity (> 95%) for the diagnosis of gallstones within the gallbladder. Accurate diagnosis of stones in the common duct is more difficult, due to overlying bowel gas. Stones can be recognized by their typical posterior acoustic shadowing. An ultrasound can also reveal signs of acute cholecystitis such as 1) thickening of the gallbladder wall, 2) pericholecystic fluid or 3) cholangitis (common bile duct dilation or intrahepatic bile duct dilation. However, biliary sludge and microcalcifications that cause biliary colic can escape diagnosis by ultrasound. Another important finding is a sonographic Murphy's sign triggered by irritation of the gallbladder with the ultrasound probe.
Plain radiographs
are seldom of diagnostic value, as only about 15% of gallstones contain
enough calcium to render them radiopaque and thus visible on plain
films of the abdomen. Pigment stones are radiolucent and not typically seen on plain x-rays.
While a computed tomography
(CT) scan can diagnose many of the other causes of intraabdominal
pathology and pain mimicking gallstone-related disease, it is less
valuable in visualizing gallstones, as bile and stones are isodense on
CT scan and difficult to distinguish. It is estimated that only 60% of
gallstones are detected by CT scan.
Biliary
scintigraphy with technetium (a HIDA scan) is an excellent test to
decide whether common bile duct and cystic ducts are patent. This
involves the administration of an isotope which concentrates within the
gallbladder, and flows into the duodenum and biliary tree allowing
visualization.
What other medical conditions can mimic gallstones?
Important conditions to consider in the differential diagnosis include:1) peptic ulcer
2) kidney stones or infection
3) hiatal hernia
4) biliary stricture or choledocholithiasis
5) Sphincter of Oddi dysfunction- biliary dyskinesia
6) hiatal hernia
7) irritable bowel
8) hepatitis
9) urinary tract infection
10) myocardial infarction
11) right sided heart failure with hepatic congestion
Post-cholecystectomy syndrome: this term signifies the subset of patients (typically 5%) who continue to complain of their original symptoms after gallbladder surgery (thus they were misdiagnosed with biliary colic). Continued studies postoperatively to evaluate for possible ulcer disease or a hiatal hernia (endoscopy and serology for the bacteria Helicobacter pylori), or biliary manometry/ ERCP should be done to assess for ampullary stenosis.
Indications for gallbladder surgery:
Gallbladder surgery can be offered for both therapeutic indications (to treat pain, infection, or cancer), or for prophylactic / preventive reasons to avoid future complications.
Therapeutic:
1) to treat right upper abdominal pain (biliary colic)
2) to treat acute active infection (acute calculous or acalculous cholecystitis, or emphysematous cholecystitis) or complications of biliary tract disease
3) to treat gallbladder malignancy- (the findings of a calcified gallbladder on x-rays known as a "porcelain gallbladder" maybe an indication for removal)
Prophylactic/ preventive:
1)
to prevent recurrent episodes of gallstone pancreatitis, cholangitis,
or cholecystitis after successful recovery from an initial episode
2) during gastric bypass surgery as the rapid weight loss after bariatric surgery can predispose to gallstone formation
3)
to prevent the development of gallstones or acute cholecystitis in a
prospective transplant recipient –particularly in the heart transplant
and bone marrow transplant populations
Which patients with gallbladder cancer can be cured?
Cancer of the gallbladder is relatively uncommon and has a very poor prognosis. This condition is associated with gallstones 70% of the time, and should be considered when an elderly patient presents with new biliary tract symptoms after the age of 65. Once diagnosed, a radical open cholecystectomy is necessary, and cure is unlikely. The 10% of gallbladder cancer patients who survive more than 5 years consist of those whose cancer was found incidentally during laparoscopic cholecystectomy for a different reason.
Can gallstones be treated without an operation?
The simplest management of symptoms from uncomplicated biliary colic can include pain medications and the alteration of diet to avoid of fatty foods. Patients who wish to avoid surgery can consider:1) Dissolution: Gallstone dissolution with ursodiol (chenodeoxycholic acid) was first reported in 1972, and can achieve dissolution of approximately half of stones less than 1 cm; however, these stones recur in about half of patients within 5 years. Given the expense, potential side effects, and lack of durability—this therapy is not regarded as effective and might be considered only in those for whom surgery is too risky or otherwise undesirable.
2) Extracorporeal shock wave lithotripsy (ESWL): This technique was introduced in the 1980s and is similar to shock wave treatment for renal stones. It is largely investigational and is of little therapeutic value as the fragments often remain in the gallbladder, requiring ursodiol treatments in an attempt to dissolve them completely. Complete elimination is seen in only 25% of patients, and as the gallbladder is not removed there is high recurrence rate of stones. This treatment has not been approved in the US by the FDA.
3) There are anecdotal reports of laxative diets using olive oil which can purge gallstones from the gallbladder, but there is no robust data to support the claims of efficacy. Moreover, this technique likely cannot discharge large stones, and the tendency of the gallbladder to form new stones will persist.
Are there any other options to surgery?
In critically ill patients who are unable to tolerate surgery, or those with recent myocardial infarction, an alternative is to drain the gallbladder with a percutaneous cholecystostomy placed under CT or US guidance. The resulting decompression controls the acute infection, though the gallstones often cannot be removed. Cholecystectomy is still advised when the patient becomes stable (perhaps in 6 weeks time). This strategy has a success rate of approximately 95%.When should I undergo operation for biliary colic?
In the setting of uncomplicated gallstone disease, surgery can be scheduled at the patient's convenience, within weeks to months after diagnosis. The patient's medical condition should be optimized preoperatively. Successful laparoscopic surgery can be performed in approximately 95% of cases, while 5% of cases will need to be converted to the traditional open approach as a result of adhesions, bleeding, abnormal anatomy, or to evaluate possible stones which have migrated into the common bile duct.Should I undergo an operation right away for acute cholecystitis, or wait until the inflammation resolves?
Standard treatment of acute cholecystitis is to begin intravenous fluids, antibiotics, pain medication, and to consider immediate surgery during the same hospitalization. Of concern is that the inflammation, edema, and adhesions around the gallbladder increase the likelihood of requiring an open cholecystectomy. The pericholecystic edema obscures the planes of dissection, and the more friable and inflamed tissues are more easily torn, resulting in blood loss, stone spillage, and postoperative bile leak. A major concern is of a greater likelihood of injury to the common bile duct. In this setting, approximately 80% of cholecystectomies can be completed laparoscopically, but 20% require conversion to the open technique to confirm anatomy and control bleeding.Thus an option is to treat the patient with intravenous antibiotics and wait for the inflammation to subside, with a plan to perform a laparoscopic cholecystectomy at a future date (often 6 weeks later) when the anatomy is perhaps less distorted. However, some patients will return with recurrent cholecystitis or more serious complications during this interval.
The timing of cholecystectomy for acute cholecystitis has thus been a long standing matter of debate. Several worldwide studies have now demonstrated that early surgical intervention offers the following advantages:
1) The incidence of technical complications is not greater with early surgery
2) The total duration of illness is reduced by about 30 days
3) The length of hospitalization is reduced on average by 5-7 days
4) Death rates are lowered by avoiding more serious complications
5) Patients often can return to work sooner
Given these significant economic, social and medical benefits – early operation is therefore the preferred approach for experienced laparoscopic surgeons and should be offered to patients at initial diagnosis once the patient is medically optimized.
Should my gallbladder surgery be attempted laparoscopically?
Generally, surgeons will first attempt cholecystectomy by laparoscopy.The following factors may represent relative contraindications to laparoscopic cholecystectomy, and do not preclude a laparoscopic approach but may represent an added level of technical difficulty:
1) previous upper abdominal scars which may limit entry into the abdomen
2) previous gastric, liver, or right colon surgery
3) obesity
4) the presence of a ventriculoperitoneal shunt
5) pregnancy, especially third trimester
6) bleeding disorders
7) end stage liver disease
8) cardiopulmonary disease which precludes general anesthesia
Conversion from a laparoscopic to open procedure in these settings should not be considered a complication, but rather the appropriate management in complex cases to maximize patient safety.
How is a laparoscopic cholecystectomy performed?
This procedure requires general anesthesia and decompression of the stomach and urinary bladder with a nasogastric and Foley catheter.1) A small umbilical incision is used to insufflate carbon dioxide to create a pneumoperitoneum; this may be done either with a special Veress needle or with a Hasson cannula. The latter method may be safer to avoid injury to the major blood vessels (aorta or IVC), which may be nearby.
2) After pneumoperitoneum of 15 mm Hg is established, a camera (laparoscope) is inserted which is connected to a light source and monitor. Three additional trocars are placed under direct vision (FIGURE), one just inferior to the xiphoid (10 mm), and two in the right abdomen ( 5mm).
3) Grasping instruments are used to retract the gallbladder superiorly and to the right to expose the triangle of Calot through which the cystic duct and artery are identified, clipped, and divided.
Alternatively,
before completely transecting the cystic duct, an intraoperative
cholangiogram may be performed to assess for common duct stones and to
confirm anatomy. The indications for cholangiography include uncertain
anatomy, known choledocholithiasis, history of jaundice or pancreatitis,
or suspected common bile duct injury. Conversion to open
cholecystectomy is advised if the intraoperative cholangiography is
ambiguous or abnormal.
4) The gallbladder is then dissected off the hepatic bed, placed into a plastic bag and removed through the umbilical or epigastric trocar site. Care is taken to avoid perforating the gallbladder during removal, which can lead to spillage of bile or stones in the abdomen and lead to intraabdominal abscess formation.
On average, the laparoscopic operation takes approximately one hour to complete. Patients typically spend a single night in the hospital, or can be immediately discharged postoperatively.
The mortality rate after elective laparoscopic cholecystectomy is usually reported in the range of 0.1 to 1%, while the major source of morbidity is related to common bile duct injury (typically reported below 1%).
How is an open cholecystectomy performed?
In contrast, an open cholecystectomy is performed through a right subcostal or vertical midline incision of 12 to 20 cm. Under direct vision, the connections between gallbladder, cystic duct, and the common bile duct are identified and separated. In uncomplicated situations, the hospital stay following open gallbladder surgery is about three to seven days.Open cholecystectomy is safe and effective, with an overall morbidity of 2 to 8% and mortality of less than 1%.
Many series of laparoscopic surgery report a similar rate of morbidity and mortality, though initial reports in the years following the adoption of laparoscopic cholecystectomy reported a common bile duct injury rate as high as 1.2%. More recent data suggests that the judicious use of intraoperative cholangiography, defining the biliary anatomy before dividing any ductal structures, and surgeon expertise have made the rate of bile duct injury equivalent between laparoscopic and open procedures.
Which patients are at risk of needing conversion from laparoscopic to an open cholecystectomy?
The following risk factors are predictive of the need for conversion:1) acute cholecystitis
2) male gender
3) older age
4) fever (temperature > 38C)
5) right upper abdominal rigidity
6) a thickened gallbladder wall seen on ultrasound
7) abnormal liver tests and elevated white blood cell count (a sign of infection)
Because the gallbladder cannot be visualized until the operation begins, the need for conversion is definitely determined only at the time of the procedure.
Complications after cholecystectomy:
The common postoperative complications after open cholecystectomy can be divided into a) biliary and b) nonbiliary complications (heart attack, wound infection, incisional hernia, stroke, pulmonary embolus).The most frequent biliary complications are:
1) Retained common duct stones. Common duct stone are present in 5% of patients undergoing elective cholecystectomy for biliary colic, and 10% with acute cholecystitis. If the stones are recognized preoperatively or postoperatively, an ERCP can be performed for extraction. But if the stones are recognized intraoperatively by cholangiogram, a common bile duct exploration and extraction are indicated.
2) A bile leak or fistula: Cystic duct leaks can occur if the clip on the cystic duct is dislodged, resulting in an intraabdominal fluid collection known as a biloma. The fluid collection can be treated by a percutaneous drain, and possible ERCP and endoscopic sphincterotomy to promote drainage into the intestine. This condition must be presumed to be a common bile duct injury until proven otherwise by further diagnostic testing.
3) Bile duct injury. The most serious and dreaded complication is a major injury to either the common bile duct or the common hepatic ducts. The duct can be partly excised, mistaken for the cystic duct, partially transected, occluded, or leak. A patient with a common bile duct injury should be transferred to a center with experience, where a repair with hepaticojejunostomy performed. Common bile duct injury is reported with a frequency of about 1 per 1000 patients after open cholecystectomy, and 1-5 per 1000 patients for laparoscopic cholecystectomy.
The minimally invasive laparoscopic approach is associated with other special complications related to trocar injuries and port site bleeding, and the learning curve associated with this newer procedure.
The major additional complication is a possible vascular (aorta or inferior vena cava) or visceral injury to the bowel during the Veress needle insertion. This risk can be reduced but not eliminated with by use of the open Hasson technique.
The management of retained common duct stones recognized intraoperatively by cholangiography during laparoscopic cholecystectomy presents three primary options:
The options are to a) perform a laparoscopic common bile duct exploration (technically challenging and dependent on surgeon expertise), b) convert to an open cholecystectomy and perform an open common bile duct exploration, or c) complete the laparoscopic cholecystectomy and perform a postoperative ERCP. Surgeon experience and patient factors and preference will determine the most appropriate course of action.
References:
1) Way LW, Stewart L, Gantert W, Liu K, Lee CM, Whang K, Hunter JG. Causes and prevention of laparoscopic bile duct injuries: analysis of 252 cases from a human factors ad cognitive psychology perspective. Ann Surg. 2003 Apr;237(4):460-9. Review.
2) Germanos S, Gourgiotis S, Kocher HM. Clinical update: early surgery for acute cholecystitis. Lancet 2007 May 26;369(9575):1774-6.
3) Stewart L, Oesterle AL, Erdan I, Griffiss JM, Way LW Pathogenesis of pigment gallstones in Western societies: the central role of bacteria. J Gastrointest Surg. 2002 Nov-Dec;6(6):891-903; discussion 903-4.
4) Lee CM, Stewart L, Way LW. Postcholecystectomy abdominal bile collections. Arch Surg. 2000 May;135(5):538-42; discussion 542-4.
5) Flum DR, Dellinger EP, Cheadle A, Chan L, Koepsell T. Intraoperative cholangiography and risk of common bile duct injury during cholecystectomy. JAMA 2003 Apr 2;289(13):1639-44.
6) Cirillo DJ, Wallace RB, Rodabough RJ, Greenland P, LaCroix AZ, Limacher MC, Larson JC. Effect of estrogen therapy on gallbladder disease. JAMA 2005 Jan 19;293(3):330-9
7) Maraescaux J, Dallemagne B, Perretta S, Wattiez A, Mutter D, Coumaros D. Surgery without scars: report of transluminal cholecystectomy in a human being. Arch Surg 2007 Sep;142(9):823-6
Useful Web sites:
1) The official statement from the Society of Gastroenterologic surgeons regarding the management of gallstones:
2) A video of a laparoscopic cholecystectomy from the National Institutes of Health:
3) A link from the American Medical Association:
4) About laparoscopic surgery:
5) A link from the American College of Surgeons:
6) Information about cholecystectomy from the American College of Surgeons:
7) A video from SAGES
8) A video of laparoscopic cholecystectomy






